Does Medicaid Pay For Braces? | How to Qualify?
Last Updated on January 18, 2024 by Lori Pace
Does Medicaid Pay For Braces? Yes, Medicaid will cover braces if medically necessary by an approved doctor. Medicaid considers your age, state, and the reason you want to straighten your teeth.
Having gone through the process myself, I want to highlight that even if your orthodontist strongly suggests that Medicaid could cover your braces, don’t forget that getting approval from your local Medicaid office is a crucial step. Trust me, I know it might seem a bit complex. Medicaid operates differently in each state, which means the coverage decisions can vary significantly. So, just a heads-up, what’s covered in one place might not be the same elsewhere.
If your income is lower, Medicaid will cover braces for you. There are special provisions in some states for children from low-income families.
When it comes to orthodontic care and Medicaid coverage, many single mothers wonder if options like Invisalign are included. Invisalign is a popular alternative to traditional braces, known for their discreet appearance and convenience. However, Medicaid coverage for orthodontic treatments like Invisalign can vary from state to state and depend on individual circumstances. To find out if you qualify for Medicaid coverage for Invisalign or other orthodontic treatments, it’s essential to check with your state’s Medicaid program and inquire about their specific guidelines and requirements.
Even if braces are required for medical reasons, coverage is tricky. You will also be disappointed if you apply for Medicaid to cover aesthetic braces.
What Are Braces?
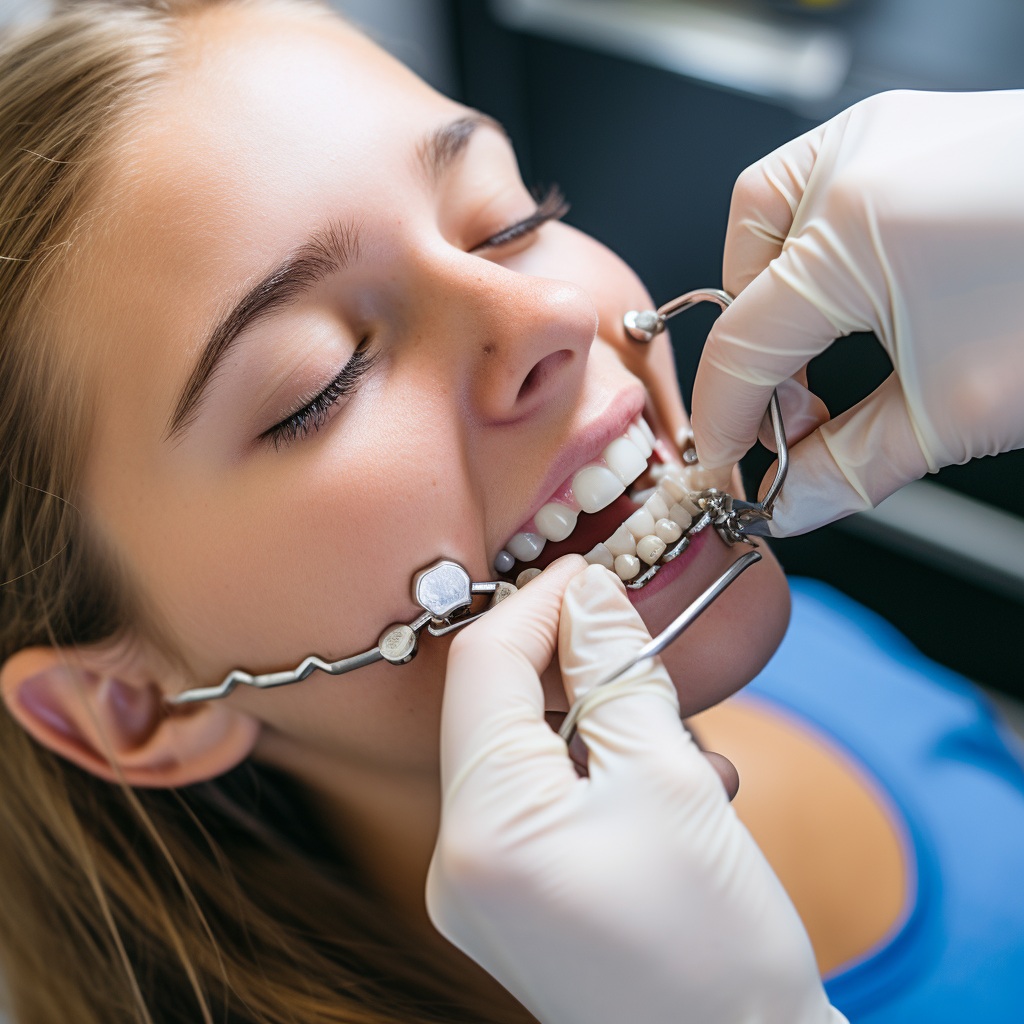
Let me break it down for you. Dental braces – those metal contraptions – are designed to fix not only those crooked smiles but also wonky bites. Trust me, they work like magic. These braces gently move your teeth to not only make them look better but also to ensure they feel better too.
Plus, they’re like a superhero for your gums and long-term oral health. You see, they even make chewing a breeze by evenly distributing the pressure across all your teeth. Usually, we associate braces with our school years, but guess what? They’re not just for kids – adults can benefit from them too. So don’t think it’s too late to straighten things out!
Braces apply pressure to the teeth and gradually move them in the desired direction. The force causes the jaw bones to shift, allowing your teeth to move. Braces can help you achieve the perfect smile.
When Does Medicaid Cover Childrens Braces?
Federal law requires that every state provides dental benefits for children enrolled in Medicaid through the CHIP (child insurance program). These benefits include:
- Routine dental check-ups.
- Restorative dentistry.
- Teeth cleaning.
- Treatment for tooth pain and infection
Medicaid does not cover orthodontic treatment for people under 21 years of age unless a doctor deems it necessary. The state-specific criteria for Medicaid coverage of orthodontic treatment vary.
Medicaid typically covers braces for children who need them to treat a disability, an injury, or a disease.
You may need braces to correct dental problems that affect normal oral functions, such as chewing and swallowing and other routine activities.
These problems could include:
- Jaw problems.
- Cleft lip or palate
- Overjet protrusions.
- Congenital defects.
- Crossbites, underbites, and overbites are severe
- Pre-existing genetic conditions can lead to missing or additional teeth.
Move your teeth slowly in the desired direction. The force will cause the jaw bones to shift in order to allow your teeth to move. Braces can help you achieve the perfect smile.
When Does Medicaid Cover Adult Braces?
Having been down this road, let me tell you how it goes. Medicaid is quite supportive when it comes to kids needing braces – that’s a relief, right? But here’s the kicker: while they do cover orthodontics for children, they’ve extended a helping hand to grown-ups too. Yeah, you heard me right! Low-income adults, pregnant ladies, and people with disabilities are now getting some love from Medicaid. But – and here’s where I raise an eyebrow – braces, unfortunately, aren’t on the Medicaid menu.
When determining whether Medicaid will cover braces for adults, medical necessity is crucial. Medicaid may pay for braces for adults who have broken or dislodged their teeth as a result of an accident.
They will cover dental care for adults with neck and jaw problems.
Medicaid will also cover the cost of teeth repositioning to correct the following conditions.
- TMD (Temporomandibular Joint Disorders) or TMJ
- Sleep Apnea
- Handicapping Malocclusions
Ensure you include information about any medical conditions that could affect your ability to get Medicaid to pay for braces. However, if you are experiencing pain or are ill, you may get approval for braces.
Medicaid can approve braces if your condition affects your normal functioning or your ability to carry out your daily routines.
What Doesn’t Medicaid Cover?
Braces can only be approved for medical reasons. The following are some of the orthodontic procedures that Medicaid will not pay for:
- The treatment of crowded teeth.
- Braces for aesthetic purposes
- If the patient does not want to maintain good oral hygiene and maintain good oral health,
Medicaid will not pay for Invisalign premium treatment options for adults and kids, as Medicaid is a mass program. However, it’s okay if you are not qualified, you can consider three alternatives for Medicaid.
How Can You Determine If You Qualify for Braces with Medicaid?
Let me share a tidbit that came across my radar. Back in 2019, the AAO (American Association of Orthodontists) dove into the nitty-gritty to define what’s medically needed in the world of orthodontics. You know, I find it fascinating how each state gets to put its own twist on things. Yep, they’re like the boss when it comes to deciding what’s on the Medicaid menu and what’s not.
Listen, I’ve been there. Wrapping your head around braces and Medicaid coverage can be a puzzle. But here’s a smart move: those consultations with a Medicaid-approved dentist? They’re golden. Seriously, they’re like your ticket to figuring out if braces are your thing and how much Medicaid’s got your back. Don’t sweat it if they’re not footing the whole bill. Dental insurance – trust me, it’s kinder on your wallet compared to the hefty medical stuff – can pitch in around 1500 bucks (or roughly a quarter of the whole deal).
Here’s a little secret I’ve learned along the way: enlisting the help of a 3rd-party dental insurance plan can be a game-changer for your wallet. Trust me, when you crunch the numbers, it’s like hitting a savings jackpot. Brace yourself – pun intended – because the out-of-pocket bill for braces can swing between 5 grand and 7 grand. But hey, if Medicaid isn’t exactly waving the magic coverage wand, worry not. There are some backup plans to keep your dental expenses in check.
- University dental clinics can provide your dental services
- No-interest financing
- Cash discounts
- Savings accounts exempt from tax
If you don’t have the funds to pay for all of your orthodontic treatment, there are non-profit programs like Smiles for a Lifetime or Smiles Change Lives that can offer braces at a reduced price.
Final Thought
Here’s the scoop: every state in the good ol’ US of A has its own set of rules about braces and what Medicaid puts on the table. It’s like a buffet, but with regulations. So, if you’re itching to know if those braces are getting a Medicaid thumbs-up, my advice? Pick up the phone or drop by your local office. Trust me, they’ve got the lowdown on what’s cookin’ in your neck of the woods.